Last week I had a patient with mild kidney disease and a high potassium. I thought that would be easy to take care of. We called around to all the pharmacies from Bangor to Ellsworth to Belfast and nobody had Kayexalate, the time-tested antidote, in stock.
It happened to be on a Tuesday night with my Suboxone group starting at 5 o’clock. The patient had been there since 4, his labs were available by 4:30.
It was 4:45 and we were almost done calling around to pharmacies. I had Autumn, my medical assistant, make some of the calls. 15 minutes left before clinic with 14 patients to see in 90 minutes (we pull them out from group therapy to check in and renew their scripts). And I had a new patient, an internal transfer but still new to me, with multiple medical problems to see before clinic.
I did what I hardly ever do: I asked Autumn to call the emergency room on my behalf and tell them that we had no choice but to send the patient over. We faxed records and lab reports and I moved on.
The ER doctor’s report was scathing. He clearly thought I had dumped on him. He didn’t do what I had thought he might do:
I hadn’t done it since I stopped doing hospital medicine a generation ago but I know you could hydrate him to help his mild acute kidney injury and coadminister glucose and insulin to lower the potassium at the same time.
Instead, the emergency room doctor gave him Kayexalate, because the hospital had it in stock. He probably didn’t know that wasn’t an option for us. I looked like an idiot to him, but that often happens in primary care.
I had gotten over my frustration and embarrassment when, this week, I had a patient on warfarin with a supratherapeutic INR and no active bleeding. I’ve never been terribly nervous about those situations but this was a high number and Up-To-Date suggested vitamin K, orally because it works faster than injectable, while obviously holding the warfarin. So, guess what, we called every pharmacy from Bangor to Ellsworth to Belfast and nobody had vitamin K in stock. The Natural Living Center in Bangor had a very low potency supplement where maybe 50 pills would be enough of a dose to make a difference.
Oune of the hospital pharmacists was available to talk to me and explained that a small bottle of vitamin K in the potency required to reverse warfarin costs about $1,000 and neither hospitals nor pharmacies want to stock them because they will lose so much money if the drug expires. What the hospitals do instead is compound an oral form from the injectable that is still expensive but less so. But a hospital can’t sell or administer to an outpatient whose primary care physician does not have privileges at that hospital. I technically have privileges at Cary Medical Center in Caribou, but that’s 200 miles north.
So this was a judgment call: Send the patient to the emergency room so she can incur the emergency room fee and have them give her an oral medication that may or may not make a difference since she had no active bleeding. Or I could bubble wrap her for a couple of days while the warfarin effect wore off.
 Today, in Van Buren, I called the small local Rexall (a historical U.S. pharmacy name) and chatted with the owner, John Hebert. He has Kayexalate in stock. This is in a town of 2,000 people. From Bangor to Ellsworth to Belfast I imagine there are 100,000 people. They don’t have outpatient access to this drug.
Today, in Van Buren, I called the small local Rexall (a historical U.S. pharmacy name) and chatted with the owner, John Hebert. He has Kayexalate in stock. This is in a town of 2,000 people. From Bangor to Ellsworth to Belfast I imagine there are 100,000 people. They don’t have outpatient access to this drug.
It’s a sad situation when potentially life-saving medications are unavailable because pharmacies don’t want to risk having them expire and go on unsold. We have automatic defibrillators in schools and shopping malls, why not some basic antidotes available, maybe even subsidized, in strategically located pharmacies?
P.S. Hebert’s is about to open a pharmacy in Bangor within the next few weeks and John has promised to stock Kayexalate there, too. And he delivers to a large geographic area…
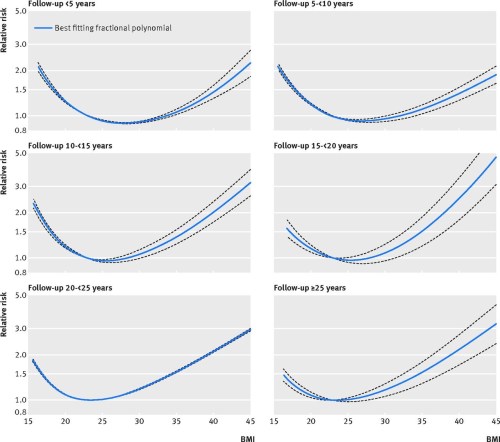 It is sobering to look at the exponential increase in death risk when BMI exceeds ideal: 20% excess risk for even average Americans, 50% greater risk at a BMI of 35 and double the risk at a BMI of 40.
It is sobering to look at the exponential increase in death risk when BMI exceeds ideal: 20% excess risk for even average Americans, 50% greater risk at a BMI of 35 and double the risk at a BMI of 40. This week,
This week, 









